
Relationship Between Weight Loss and Insulin Sensitivity

Obesity has become a global health crisis, with millions of people throughout the world fighting to control their weight. Aside from the cosmetic difficulties connected with obesity, there are serious health consequences, the most prominent of which is insulin resistance.
Table of Contents
Introduction
Insulin sensitivity is critical for maintaining appropriate blood sugar levels and avoiding type 2 diabetes. Understanding the complex relationship between weight loss and insulin sensitivity is critical for people battling obesity as well as healthcare providers and academics. In this comprehensive article, we will analyze the mechanisms and factors that relate to weight loss and insulin sensitivity, as well as the roles of nutrition, exercise, genetics, and other contributing factors.
Fundamentals of Insulin Sensitivity
The pancreas produces insulin, sometimes referred to as the “glucose gatekeeper,” which is a crucial hormone. Its principal job is to keep blood sugar levels stable and within a healthy range. When we eat carbohydrates, whether from pasta, bread, or sugary snacks, our digestive system converts them to glucose, which is then taken into the circulation. A rise in blood glucose causes a complex response.
The pancreas perceives the need to act in response to rising blood sugar levels. It causes insulin to be released into the bloodstream. Insulin serves as a key, unlocking the doors of our bodies’ cells, particularly those in muscle and adipose (fat) tissue. These cells have insulin receptors that recognize and respond to the hormone. When insulin connects to these receptors, it tells the cell to open up and let glucose in. Once inside, the glucose is either used for energy right away or saved for later use, resulting in a balanced blood sugar level.
- Insulin Sensitivity and Resistance

Insulin sensitivity refers to how well our cells respond to insulin impulses. It measures the body’s ability to absorb and utilize glucose from the bloodstream. When a person has high insulin sensitivity, their cells respond quickly to insulin’s signal and absorb glucose efficiently. This level of responsiveness is important for keeping blood sugar levels stable and for general metabolic health.
Insulin resistance, on the other hand, is the inverse of insulin sensitivity. It happens when cells become less sensitive to insulin signals. When this happens, the body must compensate for the decreased efficiency by manufacturing more insulin. In other words, insulin resistance makes the pancreas work harder to accomplish the same goal—getting glucose into cells.
The body may struggle to create enough insulin to overcome insulin resistance over time, resulting in high blood sugar levels. This continuous blood sugar rise is a symptom of diseases such as prediabetes, type 2 diabetes, and metabolic syndrome. Insulin resistance not only affects glucose metabolism, but it also contributes to a variety of health problems, including cardiovascular disease.
Relationship Between Insulin Sensitivity and Health
Maintaining optimal insulin sensitivity is critical for overall health. Diabetes affects many aspects of our health, not simply diabetes prevention. Individuals with high insulin sensitivity are well-equipped to manage their blood sugar levels. This lowers the likelihood of developing type 2 diabetes, which is defined by chronically elevated blood sugar levels caused by insulin resistance.
Furthermore, insulin sensitivity is linked to cardiovascular health. Individuals with high insulin sensitivity have lower blood pressure and are less likely to develop atherosclerosis (hardening and constriction of the arteries). These factors, taken together, lower the risk of heart disease and stroke. Aside from diabetes and cardiovascular health, insulin sensitivity regulates a variety of other metabolic processes, including lipid metabolism and inflammation, which are critical to general well-being.
Effect of Weight Loss on Insulin Sensitivity
Weight loss and better insulin sensitivity are important aspects of metabolic wellness. An extensive study has revealed that losing weight can have a significant impact on how the body responds to insulin. This weight loss-insulin sensitivity link results in not only improved blood sugar control but also a much lower risk of insulin resistance-related health problems.
Individuals who embark on a weight-loss quest are, in essence, attempting to restore their body’s metabolic balance. Excess body weight, namely adipose tissue, contributes to chronic inflammation and insulin resistance. As people lose weight, a number of mechanisms come into action, resulting in a dramatic improvement in insulin sensitivity.
- Mechanisms of Insulin Sensitivity Improvement
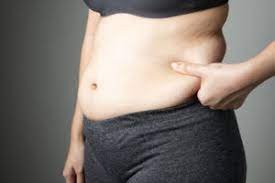
Adipose Tissue Reduction: Excess fat, particularly visceral fat (fat that collects around internal organs), is a source of inflammation. This fat has been linked to the release of inflammatory cytokines, which are signaling molecules that induce inflammation. The reduction in fat mass, particularly in the abdominal area, results in a decrease in the release of inflammatory signals as the weight loss journey develops. This decrease in inflammation creates a better environment for insulin sensitivity.
Adipose tissue is an active endocrine organ that secretes hormones known as adipokines, not only a passive reservoir for fat accumulation. Some of these adipokines are pro-inflammatory, causing insulin resistance. However, as people lose weight, their adipose tissue changes the secretion of these adipokines. This change favors a hormonal profile that promotes an insulin-sensitive environment.

Muscle Function Improvement: Weight loss is frequently accompanied by increased physical activity. Exercise not only helps with weight loss but also improves muscle function. The primary location of glucose absorption is skeletal muscle. As these muscles become more efficient at utilizing glucose, insulin sensitivity improves directly and significantly.
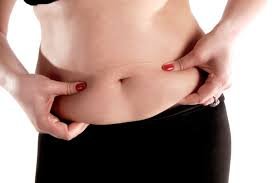
Reduced Ectopic Fat: Losing weight affects not just the fat under the skin (subcutaneous fat), but also the buildup of fat in non-adipose tissues, a condition known as ectopic fat. This form of fat has the ability to infiltrate organs such as the liver and pancreas, where it is closely linked to insulin resistance. As people lose weight, their ectopic fat deposits shrink, alleviating pressure on these vital metabolic organs and improving insulin sensitivity.
Clinical Evidence That Losing Weight Improves Insulin Sensitivity
The link between weight loss and greater insulin sensitivity is not just a theory; it has been proven in multiple clinical investigations. These studies frequently use a variety of therapies, such as caloric restriction, exercise regimens, or bariatric surgery, to promote weight loss in people who are obese and have insulin resistance.
These studies’ consistent findings leave no doubt regarding the favorable effect of weight loss on insulin sensitivity. The results are striking, whether through caloric restriction, participation in structured physical exercise, or surgical change of the gastrointestinal system. Weight loss improves insulin sensitivity significantly, making it an important strategy in the prevention and management of illnesses such as type 2 diabetes and metabolic syndrome.
Weight Loss and Insulin Sensitivity Strategies
- Dietary Strategies
Dietary methods are critical components of weight loss and insulin sensitivity improvement. The connection between what we consume and how our bodies react to it is critical to accomplishing these objectives. Several dietary approaches can be used effectively:

Caloric Deficit: Weight loss is fundamentally based on creating a caloric deficit. This entails eating fewer calories than the body burns. A caloric deficit can cause weight loss by encouraging the body to burn stored fat for energy. Simultaneously, this calorie restriction can improve insulin sensitivity by requiring effective energy management, which promotes glucose uptake by cells.

Low-Carbohydrate Diets: Reducing carbohydrate intake, particularly refined carbohydrates and sugars, is a tried-and-true technique for controlling blood sugar levels and supporting weight loss. When carbohydrates are digested, they are converted into glucose, which directly affects blood sugar levels. Cutting back on these glucose sources can help to prevent blood sugar rises, reduce insulin demand, and ultimately improve insulin sensitivity.

High-Fiber Diets: High-fiber foods, including whole grains, vegetables, and legumes, play an important role in slowing carbohydrate digestion and absorption. This, in turn, creates a feeling of fullness and helps to maintain stable blood sugar levels, minimizing the probability of overeating. Increased fiber consumption also helps to enhance insulin sensitivity.

Protein-Rich Diets: Protein is well-known for its satiating impact, which allows people to feel fuller for extended periods of time. Maintaining lean muscle mass during weight loss is critical, and a protein-rich diet does just that while also improving insulin sensitivity. Protein is also involved in a variety of metabolic activities, including blood sugar management.
Physical Activity and Exercise

Regular physical activity is an essential component of any complete weight loss and insulin sensitivity regimen. The link between exercise and insulin sensitivity is complex.

Aerobic Exercise: Aerobic exercise, such as running, cycling, and swimming, is an excellent example of aerobic exercise that can enhance insulin sensitivity. Aerobic exercise increases the capability of the muscles to absorb glucose, improving their ability to use blood sugar properly.

Resistance Training: Strength training activities are extremely beneficial for people who want to not only lose weight but also gain muscle mass while losing fat. Lean muscular tissue growth has a direct and favorable impact on insulin sensitivity.

HIIT (High-Intensity Interval Training): HIIT workouts are well-known for their ability to burn calories while also boosting insulin sensitivity. High-intensity intervals followed by short recovery times can help with weight loss and insulin sensitivity.

Changes in Lifestyle: Everyday activities can be converted into chances for physical activity. Simple changes, like taking the stairs instead of the elevator or walking instead of driving, can help you lose weight and improve your insulin sensitivity. Incorporating physical activity into daily life is a long-term strategy for health and fitness.
Weight Loss Surgery
Bariatric surgery arises as a promising treatment for weight loss and insulin sensitivity in cases of severe obesity where traditional techniques may not be effective. Gastric bypass and sleeve gastrectomy procedures have been widely researched and demonstrated to result in significant weight loss. These operations frequently result in immediate and significant increases in insulin sensitivity, making them an important alternative for people suffering from severe obesity and related metabolic issues.
- Behavioral Alterations
Weight loss and insulin sensitivity improvement can necessitate significant adjustments in behavior and cognition. These behavioral tactics for gaining and maintaining success can be quite effective:

Mindful Eating: Paying attention to hunger cues and practicing mindful eating can help with weight loss. Mindful eating encourages people to be aware of their bodies’ signals and to avoid emotional eating, which eventually aids in weight management.

Stress Reduction: Because of its impact on hormone balance, chronic stress can contribute to overeating and weight gain. Stress management strategies such as meditation, yoga, and deep breathing exercises can help people manage their stress more successfully.

Sleep Management: Inadequate sleep quality and duration can affect the hormones that regulate hunger, increasing the risk of obesity. Prioritizing quality sleep, both in terms of duration and restfulness, is critical for overall health, weight loss, and insulin sensitivity.
Factors Affecting Weight Loss and Insulin Sensitivity
- Molecular Biology

Genetic factors have an impact on an individual’s susceptibility to obesity and insulin resistance. Our genes have the ability to influence how our bodies store and metabolize fat, as well as how well they respond to weight loss strategies. Understanding one’s genetic make-up can provide useful information for optimizing weight loss strategies.
Certain genes have been linked to an increased risk of obesity and related metabolic disorders. These genes may promote fat accumulation, modify hunger and satiety signals, or influence how carbs are processed in the body. Understanding these genetic predispositions can help people make more informed food and activity decisions. For example, someone with a genetic propensity to obesity may need to watch their calorie intake more closely and engage in frequent physical activity to counterbalance their hereditary tendencies.
Furthermore, genes can influence how a person responds to various weight loss strategies. Certain diets may be more successful for some people, while others may thrive with various exercise habits. Personalized weight loss treatments based on genetic information carry the possibility of increased success in obtaining and maintaining a healthy weight, as well as improved insulin sensitivity.
- Age

Age has an impact on both weight reduction and insulin sensitivity. Individuals’ metabolisms tend to fluctuate as they age, which can impair their capacity to shed excess pounds. Metabolism slows with age, resulting in a decrease in the number of calories burned during rest. This reduced calorie expenditure can make it more difficult to generate a caloric deficit, which is a necessary condition for weight loss.
Furthermore, insulin sensitivity tends to decline with age. This age-related decrease can make it more difficult for the body to respond efficiently to insulin signals. As a result, elderly people may be more likely to develop insulin resistance, which can lead to rising blood sugar levels and an increased risk of metabolic illnesses.
Given the impact of aging on metabolism and insulin sensitivity, it is becoming increasingly vital for people to focus on maintaining a healthy weight and engaging in regular physical activity as they age. These lifestyle choices can help to reverse the metabolic changes that come with aging, encouraging improved overall health and lowering the risk of insulin resistance.
- Gender
Gender variations are significant in how the body stores and burns fat. Men and women may react differently to different weight loss regimens and have variable insulin sensitivity. Women’s hormone swings, particularly during menopause, can have a substantial impact on weight management and insulin sensitivity.
Fat distribution patterns differ between men and women. Men prefer to store fat in their abdomens, but women tend to store fat in their hips and thighs. When implementing weight loss procedures, these changes in fat storage might influence how much weight is lost and where it is lost.
Hormonal changes, such as those women experience during their menstrual cycle, pregnancy, and menopause, can have an impact on appetite, cravings, and how the body processes and stores fat. These hormonal changes might provide specific problems for women during their weight loss endeavors, necessitating the need for specialist tactics and support.
By learning about these gender-specific traits and making changes to weight loss plans as needed, people may be able to reach their goals more easily and avoid problems that can come up because of differences in metabolism and hormones between men and women.
Note: There might be affiliate links mentioned here. We may receive a commission if you purchase a product through an affiliate link. There is no additional charge for you. Please do your own research before making any online purchases.
- Hormonal Factors

Hormonal abnormalities, such as those caused by polycystic ovarian syndrome (PCOS) or thyroid diseases, can have a significant impact on a person’s ability to lose weight and alter insulin sensitivity. Addressing underlying hormonal imbalances is frequently required for optimal weight loss and insulin sensitivity.
PCOS, for example, is a common hormonal condition that is frequently related to insulin resistance and weight gain in women. PCOS’s hormonal irregularities can make it difficult to lose weight and aggravate insulin resistance, making it a particularly tough condition to manage.
Thyroid diseases, such as hypothyroidism, can impede metabolism and make creating a calorie deficit for weight loss more difficult. To restore thyroid function and improve metabolism and insulin sensitivity, hormone replacement treatment or medication may be required.
To deal with hormonal changes in these situations, people often need a multifaceted approach that includes medical help, changes to their lifestyle, and specific dietary advice. This helps them reach their weight loss goals while also making their bodies more sensitive to insulin.
Challenges to Weight Loss and Improved Insulin Sensitivity
- Set Points and Plateaus

Weight reduction journeys frequently hit stumbling blocks, where progress appears to stagnate despite constant attempts. The body’s set point, which is a natural weight range that it tries to maintain, has an impact on these plateaus. When people reach a specific weight, their bodies may oppose further weight reduction, making it difficult to push over this barrier.
Overcoming plateaus necessitates a calculated strategy. Diet and exercise routine modifications are frequently required. Changing your caloric intake, varying your workout routines, or integrating more difficult workouts will help your body break through the plateau. During this phase, it is critical to be patient and consistent, as breaking through a plateau may be extremely rewarding in terms of both weight reduction and enhanced insulin sensitivity.
- Adherence and Longevity

Maintaining long-term adherence to solutions is one of the most common obstacles to weight loss and improved insulin sensitivity. Maintaining weight loss and insulin sensitivity improvements requires long-term adjustments in food and exercise behaviors. Many people struggle with the long-term commitment required to live a healthier lifestyle.
Sustainability is frequently achieved by incremental, realistic modifications and the establishment of attainable goals. It is critical to have a balanced, pleasurable diet and exercise program that can be incorporated into one’s lifestyle. These modifications must be viewed as a long-term commitment rather than a temporary remedy. Having a support system in place, such as friends, family, or a healthcare professional, can also provide inspiration and accountability.
- Psychological Aspects

Emotional eating, body image concerns, and stress can all greatly hamper both weight reduction and insulin sensitivity improvements. Emotional eating, in particular, can lead to an excess of unhealthy foods, impeding weight loss efforts. Body image concerns can have an impact on self-esteem and motivation, impacting weight reduction plan adherence.
Taking care of these psychological issues is critical for long-term success. Individuals can benefit from therapy or counseling in order to better cope with emotional eating and stress. Increasing self-esteem and cultivating a good body image can improve motivation and self-care. A comprehensive approach to health that considers the psychological components of weight management can result in more long-term, effective weight loss and insulin sensitivity improvements.
Emerging Research and Future Directions
- Personalised Approaches

Personalized techniques are gaining relevance in the shifting landscape of weight management and insulin sensitivity enhancement. Advances in genetics and customized medicine have made it possible to tailor interventions to a person’s specific traits, enabling a more effective and efficient road to weight loss and insulin sensitivity.
Personalized techniques acknowledge that each person’s genetic make-up, metabolic profile, and lifestyle are distinct. Healthcare specialists can build weight reduction and insulin sensitivity regimens that are precisely tailored to an individual’s needs by assessing genetic markers, medical history, and current health conditions. Specific food suggestions, exercise routines, and targeted medicinal interventions may be included in these individualized plans.
- New Treatments
The landscape of weight reduction and insulin sensitivity medicines is constantly changing, with new techniques being investigated. These newer medicines attempt to combat obesity and insulin resistance more effectively, providing new hope for people dealing with these issues. Among the promising paths are:
Modulation of the Gut Microbiome: The gut microbiome, a collection of bacteria in the digestive system, plays an important role in metabolism and energy control. New research is looking into ways to manipulate the gut flora to assist weight loss and insulin sensitivity.
Gene Therapy: Advances in gene therapy are investigating the prospect of targeting specific genes linked to obesity and insulin resistance. This innovative technique has the potential to treat the underlying genetic causes of many diseases.
New Medications: Researchers are working on new medications that will boost insulin sensitivity. These drugs are designed to improve the body’s reaction to insulin, making it more effective at controlling blood sugar.
Telemedicine and Digital Health

The digital revolution is reshaping the healthcare scene, making it more accessible and convenient than ever before. Telemedicine and digital health technology have the potential to change weight loss and insulin sensitivity management. These innovations provide:
Remote Access: Individuals can get weight loss programs and diabetes control support remotely, removing the need for in-person sessions and allowing for greater scheduling flexibility.
Increased Engagement: Digital tools like smartphone applications and wearable devices allow people to track their progress, get real-time feedback, and stay motivated on their weight reduction and insulin sensitivity journeys.
Expert Advice: Telemedicine enables people to interact with healthcare professionals and specialists online, allowing them to receive expert advice and support from the comfort of their own homes.
- Social and Community Support

Recognizing the value of social and community support in health and wellbeing, community-based weight loss programs and social networks are gaining popularity in the quest for better weight management and insulin sensitivity.
These programs provide participants with a sense of belonging, drive, and accountability. Being a part of a supportive community can make a huge impact on weight loss plan adherence. Group-based activities, such as group exercises, nutritional education seminars, or online forums, offer individuals a network of like-minded others who share similar aims and problems, whether in-person or virtually.
FAQs
What is the connection between losing weight and improving insulin sensitivity?
Weight loss has a significant effect on insulin sensitivity. Losing weight can improve how the body responds to insulin, resulting in better blood sugar control and a lower risk of insulin resistance-related health problems.
What is insulin’s function in the body?
The pancreas produces insulin, which regulates blood sugar levels. It facilitates the entry of glucose into cells, where it is either used for energy or stored, keeping blood sugar levels within a safe range.
What exactly is insulin sensitivity?
Insulin sensitivity is the efficiency with which cells respond to insulin signals, allowing for efficient glucose uptake. Insulin sensitivity supports blood sugar stability and general metabolic health.
What exactly is insulin resistance?
Insulin resistance develops when cells become less sensitive to insulin and require more insulin to achieve the same glucose absorption. It causes high blood sugar levels and is linked to illnesses such as type 2 diabetes and metabolic syndrome.
How does losing weight enhance insulin sensitivity?
Weight loss reduces adipose tissue, particularly visceral fat, which reduces inflammation and improves insulin sensitivity. It also influences the release of pro-inflammatory hormones from adipose tissue, enhances muscle function, and decreases ectopic fat.
What are some dietary strategies for increasing insulin sensitivity?
Caloric deficit, low-carbohydrate, high-fiber, and protein-rich diets can all help you lose weight and increase your insulin sensitivity.
What effect does exercise have on insulin sensitivity?
Aerobic exercise, strength training, HIIT, and commonplace activities such as walking can increase insulin sensitivity by boosting muscle glucose uptake and decreasing fat mass.
When should you consider bariatric surgery for weight loss and insulin sensitivity?
When standard approaches fail to alleviate extreme obesity, bariatric surgery, such as gastric bypass or sleeve gastrectomy, is explored. It frequently results in quick weight loss and improved insulin sensitivity.
What role does genetics play in weight loss and insulin sensitivity?
Genetics can influence an individual’s proclivity to obesity as well as how they respond to weight loss programs. Understanding genetic characteristics can aid in the development of weight loss therapies.
What obstacles can people confront when trying to lose weight and enhance their insulin sensitivity?
Plateaus, adherence, and durability, as well as psychological issues such as emotional eating and stress, can all stymie progress. Overcoming these obstacles necessitates changes, perseverance, and psychological support.
Conclusion
The connection between weight loss and insulin sensitivity is intricate and nuanced. Weight loss has a significant impact on insulin sensitivity, with mechanisms involving changes in adipose tissue, muscle function, and the lowering of ectopic fat. Dietary adjustments, exercise, behavioral changes, and, in some situations, medicinal interventions are all part of weight loss and insulin sensitivity strategies. Individual factors such as heredity, age, gender, and hormone imbalances all influence how a person responds to weight loss efforts.
Plateaus and psychological issues are common obstacles to attaining weight loss and better insulin sensitivity, but they can be overcome with patience and support. The future of this field’s research and interventions looks bright, with an emphasis on tailored methods, innovative therapies, digital health technologies, and community support.
Understanding the complex relationship between weight loss and insulin sensitivity is critical not only for those suffering from obesity and insulin resistance but also for healthcare professionals and researchers battling the global epidemic of type 2 diabetes and related metabolic disorders. As we continue to decipher the underlying mechanisms and devise more effective solutions, the prospects for enhancing the health and well-being of millions of people throughout the world appear brighter than ever.
Disclaimer: The information provided in this article is for educational purposes only and should not be considered as a substitute for medical advice. Consult a healthcare professional before implementing any home remedies or making significant changes to your lifestyle.






